Learn
All you need to know about Palliative Care
WHAT IS PALLIATIVE CARE
Palliative care makes the unthinkable an experience!
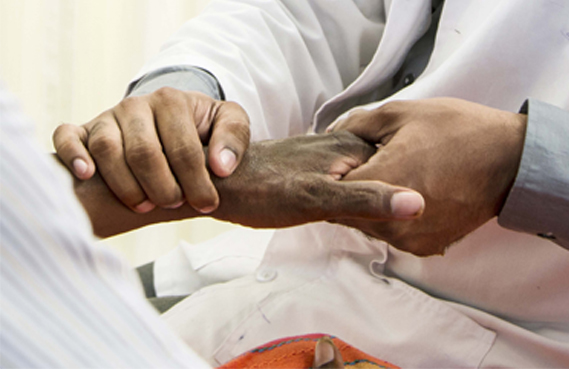
Palliative care, a stream within organized medical care, follows a multidisciplinary approach to relieve a patient with a serious illness from the distressing and painful symptoms of their diagnosis. The disciplines that come together in palliative care include doctors, nurses, anesthetists, social workers, counsellors, dieticians, physiotherapists, occupational therapists and when needed lawyers too who will support the patient and their families with the aim of enhancing their quality of life.
Palliative care provides holistic care fulfilling the patients’ emotional, spiritual, psychological and financial needs. The patient is any individual - young or old – whose daily life and ability to perform activities has been limited by the distress they experience due to symptoms of their disease.

These symptoms include pain, anxiety, difficulty sleeping, loss of appetite, depression, fatigue, constipation, nausea, shortness of breath amongst others. Palliative care focuses only on alleviating distressing and painful symptoms of both curable and non-curable diseases.
Palliative care is breaking the age-old mindset that disease and pain are inseparable. It is breaking its way through the orthodox order of the day wherein decisions are made on behalf of the patient.
It is establishing and reiterating the patient’s right to choose and live a quality life, which for some could be fleeting.

Palliative Care is defined as “an approach that improves the quality of life of patients and their families facing problems associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual.” (as defined by WHO)
PALLIATIVE CARE FOR YOU
If you are here, you should be informed better!

Palliative care enhances quality of life. But just how is that done?
-
Alleviating symptoms of distress and pain allows the patient and family to enjoy life and perform daily activities which were otherwise limited.
-
Financial demands and strains are greatly reduced because of its simple and cost-effective approach and services provided.
-
The patient and family are met within the framework of their own comfort.
-
In addition to enjoying the company of each other in their comfort zones, the patient and family benefit through a robust support system of the palliative care team.
-
The patient has the opportunity to dream and continue to live a fulfilling life.
Allow us to help enhance your quality of life! A comprehensive understanding of ‘our services’ will help you make the right decision of giving your loved one the comfort and pain-free experience they desire.

Six out of nine million persons who die each year in India are in need of Palliative care! There are over 5 million people needing palliative care each year in India. But services available cater to only a mere 1% of India’s total population of 1.3 billion. There are 908 palliative care centers in India of which 804 centers are concentrated in the pioneer state of Kerala.
PALLIATIVE CARE IN INDIA
The demand is enormous but unmet!
1986

1986 - 1993
Very first hospice in mumbai 1986, Two more branches in Delhi and Goa in 1991 followed by Pain and Palliative Care Society (PPCS), Calicut.


1994 - 1995
Centeres in Assam, Bangalore, Chennai, Delhi. Palliative care services included in pre-existing pain management centere. Proposal Submitted to Golfor simplification of Narcotic Drugs and Psychotropic Substances Act (1985).

1998 - 2005
Model rule laid by Golfor modification of existing state regulations in 1998. In 2003 Pallium India Created to improve access to palliative care outside Kerala. Later in 2005 Pallium India submitted a representation to Government of Kerala and to GoI to frame ‘Palliative Care Policy’.


2006 - 2008
In 2006 Committee to work on National Policy for Palliative Care formed by GoI. In 2007 Palliative care activists approached the Supreme Court of India and appealed for central and state level palliative care policies. In 2008 Government of Kerala declared a palliative care policy integrated into health care.


2009 - 2012
In 2009 Human Rights Watch recommended INCB to plan a fact finding mission to India, with the availability of controlled substances for medical and scientific purposes as one area of focus. In 2010 Medical Council of India accepted palliative medicine as a medical specialty and announced a postgraduate course in the subject. In 2012 the first Doctor of Medicine (MD) course was started at the Tata Memorial Hospital in Mumbai.


2013 - 2015
In 2013 Meeting to create a palliative care strategy for the country’s five-year plan.In 2014 NDPS Amendment Act was passed which transferred the powers for legislation on “essential narcotic drugs” (ENDs) from the state governments to the central Government. In 2015 GoI concluded the process with notifications regarding the rules to be followed by the state governments.
Subscribe to our Newsletter
Contact Us
Call us at +91-9943075607 or
Email Us at info@sharonpalliativecenter.org
18,Tanmag Road, 636008 Salem,
India
Follow Us
Accredited to





